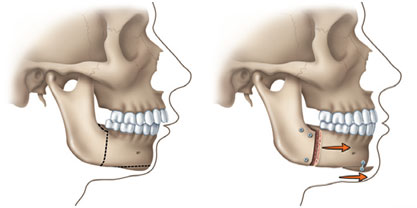
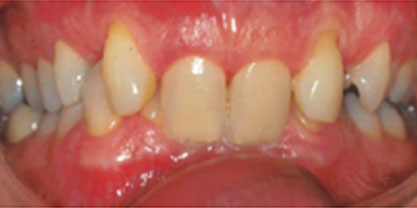
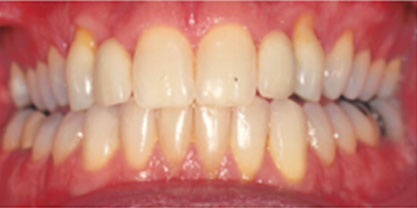
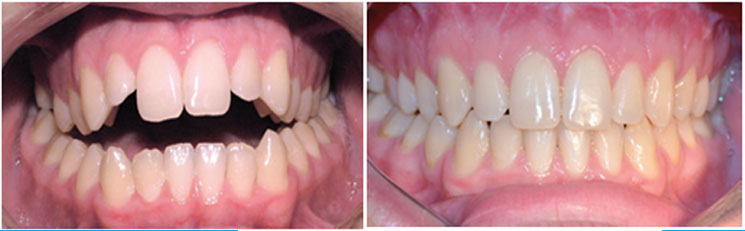
Orthognathic surgery is an operation to reposition the jaws. (Ortho means straighten, gnathia means jaw in Latin). The operation aims to correct imbalance between the upper and lower jaws which will enable the teeth to bite together correctly; this also has the benefit of balancing and enhancing the facial appearance.
It is also termed as corrective jaw surgery.
It is not always possible to correct your teeth and how they bite together using only orthodontic treatment (Braces). This is because the bones of your face and jaws, in which the teeth sit, may be out of balance with one another. (For example, you may have a larger/smaller lower jaw and a normal sized upper jaw or vice versa). Orthognathic surgery is able to correct these bony discrepancies and balance the shape, function and appearance of the face.
People who may benefit include those with an improper bite resulting from misaligned teeth and/or jaws. In some cases, the upper and lower jaws may grow at different rates. Injuries and birth defects may also affect jaw alignment. While orthodontics can usually correct bite, or “occlusion,” problems when only the teeth are misaligned, corrective jaw surgery may be necessary to correct misalignment of the jaws.
Following are some of the conditions that may indicate the need for corrective jaw surgery:
It is important to use braces to move the teeth to make sure that they will meet together correctly after the operation. Usually, the orthodontist will fit the braces months before surgery. They are worn for up to 6 months afterwards until the teeth are finely adjusted and stabilised. Lastly, there will be a period when a removable retainer brace is worn that holds the teeth in their new position.
In total, treatment may take about two and a half years, with the surgery at about 18 months from the start of orthodontics. Please note that the period of orthodontic treatment is lengthened by missed appointments and any breakages of the brace.
The main problem after surgery is numbness and swelling rather than pain. Everybody is different, but most patients find the swelling is at its worst 36-48 hours after the surgery and it gradually goes down over the next fortnight. Your final appearance takes several months to fully emerge as the shape of your face adjusts. Patients may find it uncomfortable breathing through their nose and may have a sore throat after surgery for a few days. In general older patients seem to find these symptoms worse and take longer to get over the operation than younger patients.
This depends on the individual but most patients stay in hospital for two or three nights after surgery. People vary in their speed of recovery, but you should consider taking two to three weeks off from whatever you normally do.
The operation is all done from inside the mouth, so there are no external scars. The jawbones are repositioned into a new but pre-planned position and secured by tiny plates and screws, which remain under the gum. The teeth are not normally wired together but small elastic bands are used between the top and bottom braces to guide the teeth into their new bite.
Before your surgery, orthodontic braces move the teeth into a new position. Because your teeth are being moved into a position that will fit together after surgery, you may at first think your bite is getting worse rather than better. When your Oral & Maxillofacial surgeon repositions your jaws during surgery, however, your teeth should fit together properly.
As your pre-surgical orthodontic treatment nears completion, additional or updated records, including x-rays, pictures and models of your teeth, may be taken to help guide your surgery.
Depending on the procedure, surgery may be performed under general anesthesia in a hospital. Surgery may take from one to several hours to complete.
Your surgeon will reposition the jawbones in accordance with your specific needs. In some cases, bone may be added, taken away or reshaped. Surgical plates, screws, wires and rubber bands may be used to hold your jaws in their new positions.
After surgery, your surgeon will provide instructions for a modified diet, which may include solids and liquids, as well as a schedule for transitioning to a normal diet. You may also be asked to refrain from using tobacco products and avoid strenuous physical activity.
After the surgery the orthodontic treatment will be continued for a period of 4 to 6 months. This is to make fine and finishing movement of teeth to provide you a perfect bite.
The mouth opens and closes normally, even on the day of surgery, but the opening is limited by the elastic bands and swelling. You will be encouraged to eat and drink from the first day and gradually progress from liquids to soft food and then to your normal diet over the next few weeks.
This is usually a very safe procedure which is carried out regulary in this hospital by specialised and experienced clinical staff. Complications in this type of surgery are, fortunately, rare and may not apply to you but it is important that you are aware of them.
Numbness - The lips will be numb immediately after the operation, similar to the sensation of an injection of local anaesthetic at the dentist. The upper lip recovers quickly. The lower lip is much more variable and may take 6-9 months to get its normal feeling back. Very rarely sensation never completely returns.
(The lip still looks and moves normally and only exceptionally does it bother patients).
Infection - The tiny fixing plates are usually left in place permanently. In less than 10% of cases the plates may have to be removed if they become infected but this is usually after they have done their job.
Re-adjustment of the bite - In rare circumstances the bite may require adjusting. This sometimes occurs when the patient wakes up from the relaxed state of the anaesthetic and the strong jaw muscles move the bite. Minor changes of a millimetre or two can be corrected during postoperative orthodontic treatment phase, in rare cases a second operation to adjust the plate fixation may be necessary.
Relapse - means movement of jaw bones to their old position. With most patients significant relapse is not a problem. However those who are having complicated surgery (movements of 10mm or more in one jaw, patients previously having had a cleft palate, or those with a particularly unusual bite) a relapse can occur. If relapse does occur, it is exceptionally rare for this to be significant.
You will almost certainly look different to some degree; quite how different depends on the extent of your original problem and how much the jaw(s) have had to be moved. The doctors generally decide the jaw movement direction and amount preoperatively and the expected change in your appearance can be predicted. Nowadays they even can show you that how will you look after surgery with the help of certain software. The vast majority of patients are delighted with the Orthognathic surgery aims to balance the bony framework of the face, so that all the features are in proportion to one another, producing a pleasing facial appearance and teeth that chew properly.
YES, don’t have the operation. Nobody wants you to have the operation unless YOU want it. There are always new developments in medical Science, you can discuss with your doctor regarding all the treatment options but, at the moment, this is the most successful and reliable method of correcting the facial appearance in those patients who have jaw discrepancies beyond the correcting limits of orthodontic treatment.
Some of the bone in the upper tooth-bearing portion of the jaw is removed. The upper jaw is then secured in position with plates and screws.
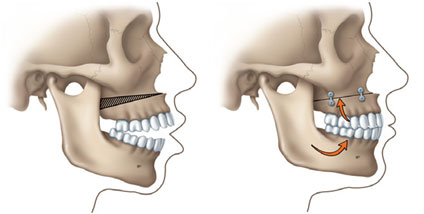
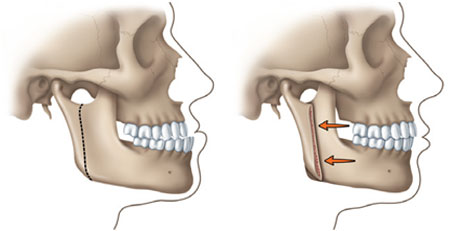
Correcting a Protruding Lower Jaw:
The bone in the rear portion of the jaw is separated from the front portion and modified so that the tooth-bearing portion of the lower jaw can be moved back for proper alignment.
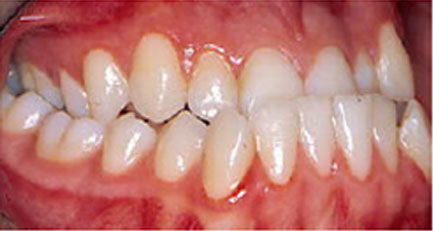

Correcting a Receding Lower Jaw or "Weak Chin":
The bone in the lower portion of the jaw is separated from its base and modified. The tooth-bearing portion of the lower jaw and a portion of the chin are repositioned forward.